(Title image: Photo by Nick Fewings on Unsplash)
Yep, this is another installment of “I had another oncologist appointment today”. This time I’m marking seven years since completing my chemo treatment, which I can assure you at the time was a very happy event…
…marred only by that little nail infection a few weeks later. But don’t go there unless you have a strong stomach.
Regardless, I had a great meeting with my oncologist. The concern now is about whether I’m experiencing anything cancer-related, either long-term side effects or—perish the thought—a recurrence. Today the answer was neither.
We talked about the recent death of my father…and that’s pretty much the way the appointment went–catching up on the last six months. Naturally, I forgot to tell him about a bunch of the other concerns I had, little weird things in my body. But really, they’re not unusual given what I’ve gone through.

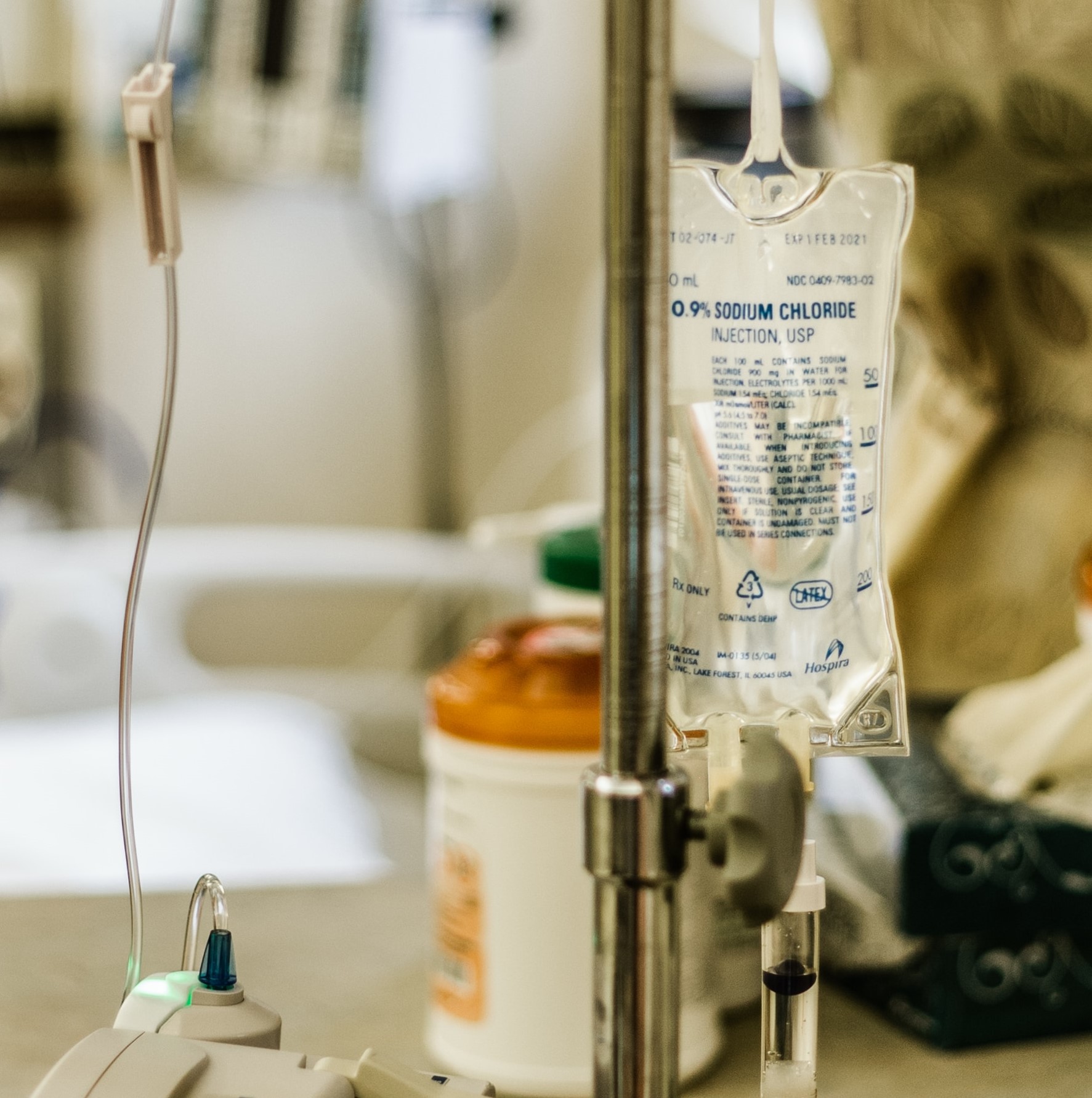
(Photo by LOGAN WEAVER | @LGNWVR on Unsplash)
We did, however, discuss how it takes a little while to get used to all those sensations in your body. After cancer, I was on high alert. My medical team was asking detailed questions about what I was feeling, and as a result, I was laser-focused on every twitch and twinge…and maybe some that I just imagined. At one point, I was sent for a brain MRI because of what I feared were serious cognitive issues. But in reality it was anxiety, not a tumor.
Seven years out, however, you kinda get expect all those funny sensations and don’t interpret them as being dangerous anymore. Even the heart palpitations that I would get from time to time…yeah, I still get those, maybe once a week, maybe a couple of times a month. But they only last a handful of seconds and I no longer think that my heart is failing (especially not when I can turn around and do a HIIT workout). I haven’t been back to the cardiologist and my oncologist agrees that it’s not necessary.
He asked if I wanted to come back in six months. Sure, I like being back in the Cancer Center as *NOT* a cancer patient. It’s nice being there and remembering doing jigsaw puzzles in the radiation oncology waiting room, or even feeling well-taken-care of after my treatments were done. There ARE positive memories in a place that you’d think would only be negative.
That can change very quickly, of course. But for the time being, I’m feeling happy.