More than two years after finishing chemo, after being afraid my hair would not grow back, and after being delighted with the way it did…I’m experiencing follicular drama, once again.
Once chemo was over, my sleepy follicles took their time getting roused into action. To say that I worried would be an understatement. I was still caught up in the unfairness of being smacked down by breast cancer. Confronting the possibility that after enduring the nastiness of cancer treatment, I might not get my hair back? That was too much.
Well, if you’ve read my posts on hair, you’ll know that my hair finally did come back. And there was much rejoicing.
And that’s where my hair posts stopped. But as happens with these kinds of things, that wasn’t the end of the story.
While still bald, I had been fed reassuring anecdotes by well-meaning supporters about hair coming back even better than before, lush locks that served as well-deserved rewards for undergoing the anxiety and strain of cancer diagnosis and treatment.
But as much as cancer patients feel like they don’t know what’s going on, those around them have even less of an idea. They want you to “stay positive” at all costs, so they overload you with lots of good news.
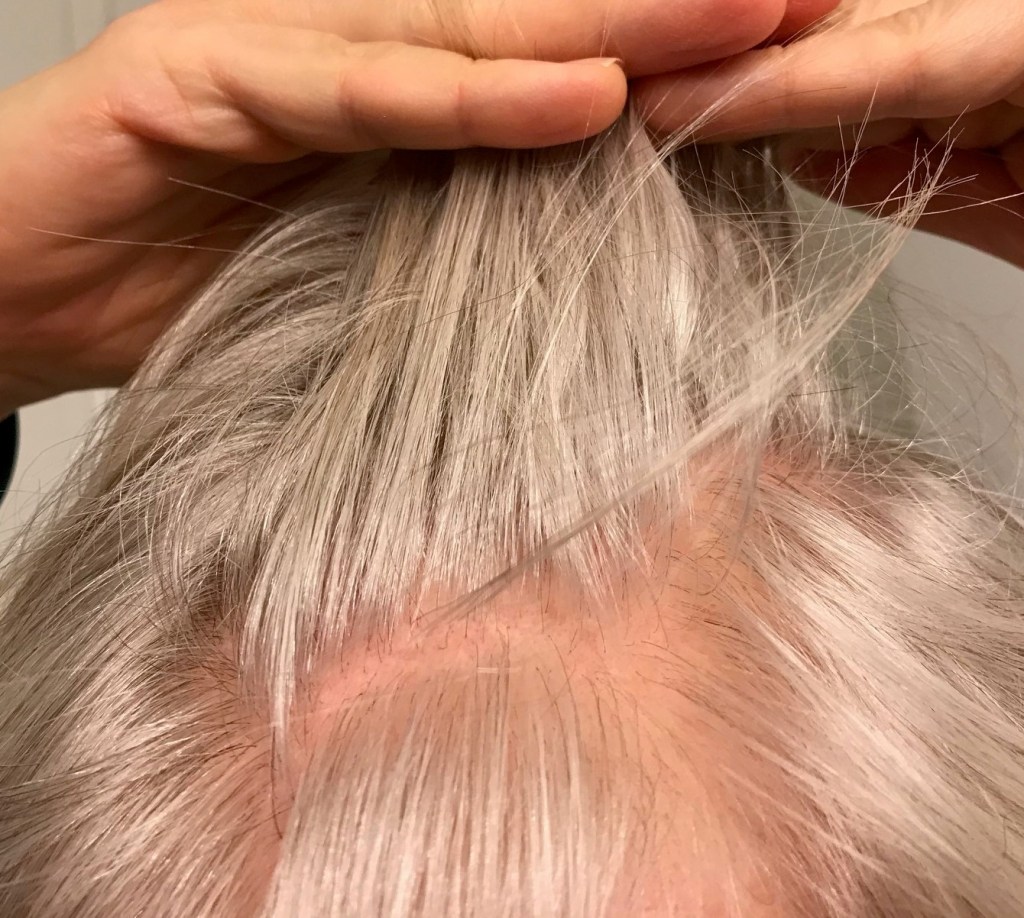
By now you can probably guess where I’m going with this. Because in Spring 2019, things started changing. Within a few months, my uber-cool spikey rockstar hair lost fullness as my strands thinned. Then, I saw “bald spots”.
So, let me explain how I define “bald spots”: these areas have hair, but due to the color (um, WHITE) and thinness, the hair seems translucent, even transparent. And along the part? You can’t see the roots well at all.
My reward for enduring cancer is invisible hair.
My hairstylist confirmed that the hair that comes back in after chemo is different from the hair that eventually settles in. And mine had settled.
Tamoxifen also played a role, since choking off estradiol and moving into menopause will age both you and your hair, particularly if you are premenopausal going into treatment, as I was. So this should have been expected, but in the hustle and bustle of all the other little things, like, oh, wondering if you’re going to survive the ordeal, no one really talks about the fact that there will be other changes that take place.
And now, I’ve been off tamoxifen for almost six weeks, but can’t tell whether there’s been any regrowth, not that I expect any. I meet with my oncologist this Tuesday and you can bet your panties he’s going to prescribe an aromatase inhibitor for me, so the pharmaceutical depression of estrogen will continue.
I am dealing. Mostly. Am I happy about this? Of course not. The last few years have felt like running a gauntlet of misery, but one where I’m only hobbled and not completely taken out. Given that, I’m ashamed of complaining, as there are many others doing so much worse. But not ashamed enough to stop writing about it, as this is my reality and it affects me. If I’m going through this, there’s a good chance that many others are too.
I’m supposed to be moving on and leaving cancer behind me, right? But like an annoyingly nosy neighbor, it keeps waving at me through my kitchen window, reminding me that it’s living next door.



















