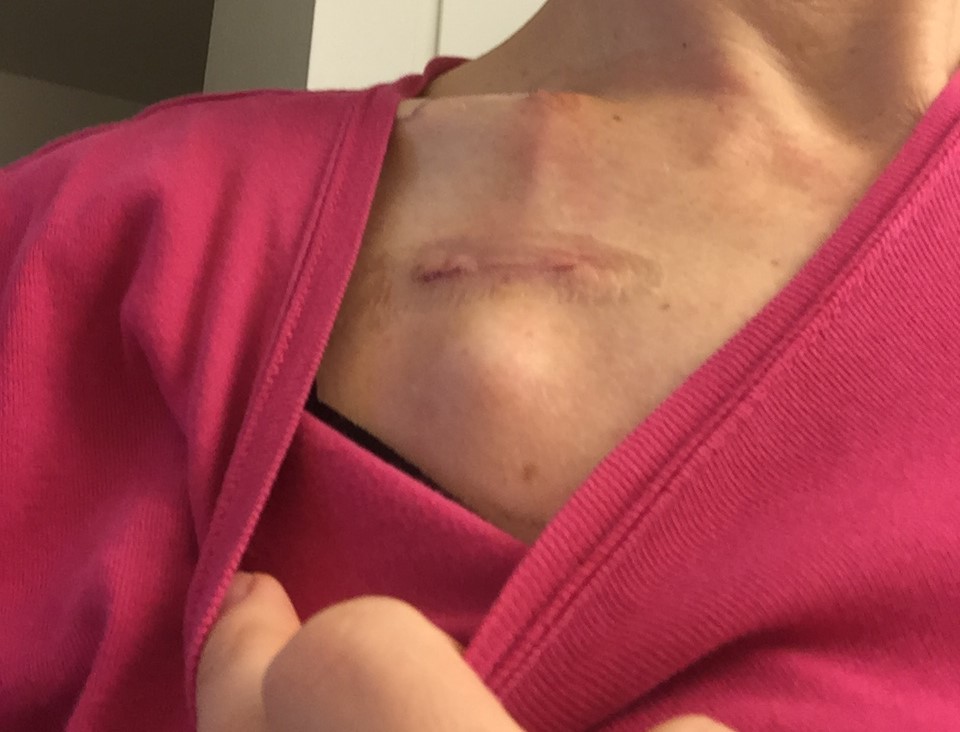
When is a “chemo port” not a chemo port? When it’s a heart rate monitor. Except that my emotional brain can’t tell the difference.
For anyone unfamiliar with cancer chemotherapy, a chemo port, or subcutaneous implantable catheter, is a device implanted under the skin (usually on the chest) that is accessed during an infusion to enable easy mixing of the chemo drugs with blood within a major blood vessel. This avoids a good deal of injury to any smaller blood vessels, were you to get chemo drugs via an IV to your arm. (For more info, see this post.)
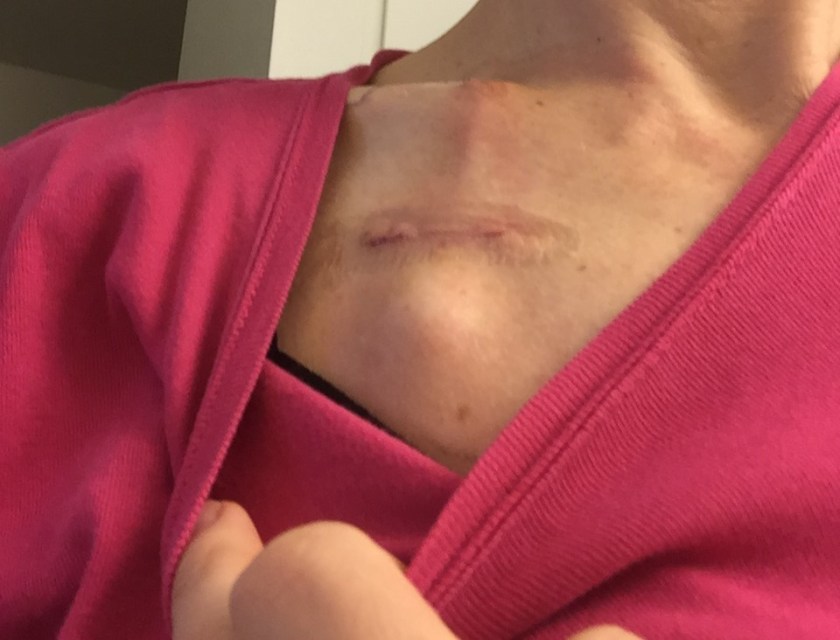
As much of a blessing as the chemo port is, having a foreign object pushing up from the chest wall under your skin can give “Alien” (as in the movie) vibes. For me personally, the implanted chemo port was more psychologically taxing than I anticipated, and as soon as all my infusions were done, which took a year, I had it taken out ASAP.
So almost three years after its removal, the chemo port is spooking me again, this time in the form of an extended Holter monitor for continuous heart rate recording, which I’ll have on for almost two weeks. It’s taped to the skin in a fancy patch that you can exercise and shower in, and supposedly you forget that you’re wearing it and go on your daily routine as normal.
But for me, it’s bringing up the spectre of chemo port, and memories of discomfort and pain I felt having that bulge stretching my skin of my chest. I chant my mantra of “it’s ON, not IN” in an effort to distinguish between the port and monitor, but the longer than it stays on, the more anxiety I feel about it.
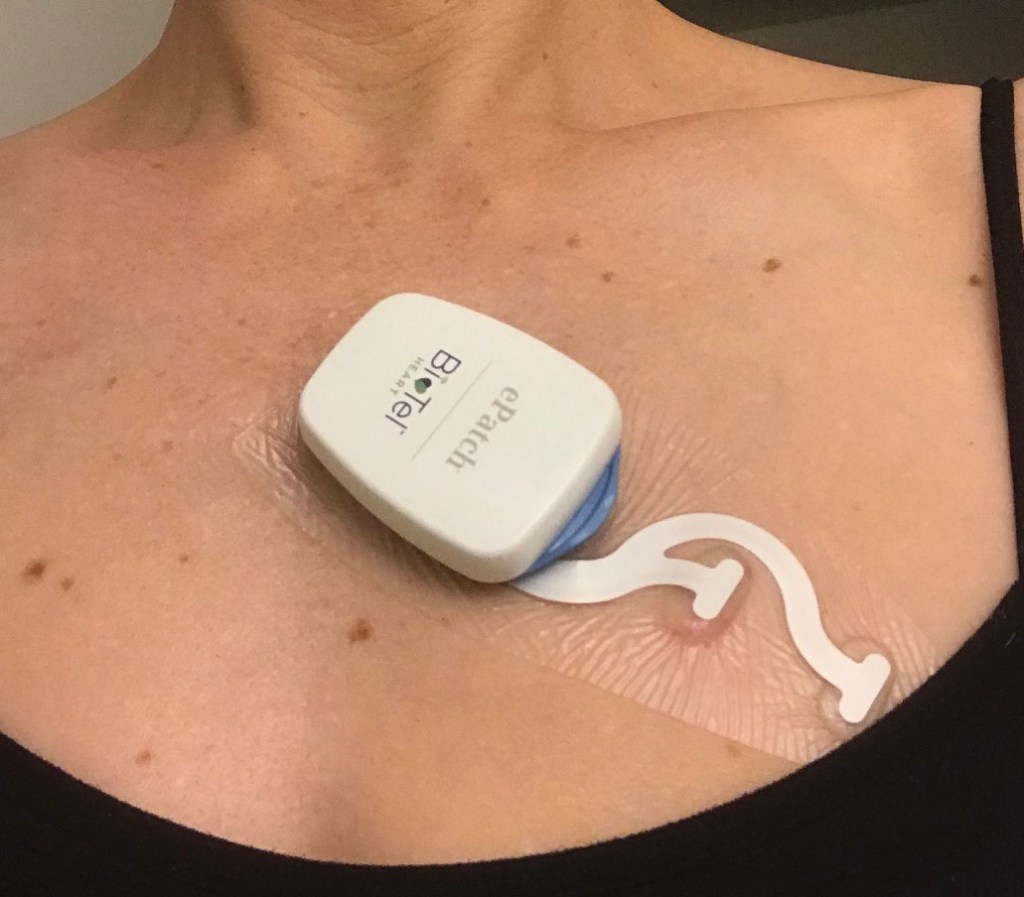
All those emotions about the lack of control over my own body, feeling so abnormal and outwardly looking “sick” (not to mention fear of death) are rushing back. The Holter monitor peeks up from the neckline of my shirt, hooks my car’s seatbelt and often seems to be in the way. I find myself moving away from other people in fear of having them knock it or hug me too tightly and cause pain, even though the monitor doesn’t deserve the same apprehension that the port did.
I’m removing the Holter patch today and sending it back for analysis, so that’ll be a big relief. But the power of this reaction is another reminder of the depth of fear that the cancer experience placed within me.
~~~~~~~~~~~~~~~~~~~~~~~~~
So why am I wearing the heart rate monitor anyway? I was having little cardiac “episodes”, particularly over the last year, and this was one of the (many) reasons for discontinuing aromatase inhibitors. Mainly these were sensations of skipped or extra beats or an odd “fluttering”. I’ve already had an EKG and echocardiogram, neither of which apparently showed anything abnormal (I haven’t received a final report of my echocardiogram but had been told that the cardiologist would contact me if he found anything problematic, and it’s been a week and a half, so I’m guessing everything’s okay?).

The Holter monitor was the last step in looking for arrhythmias or similar issues. And wouldn’t you know it? The further I’ve gotten from stopping aromatase inhibitors, the fewer episodes I’ve experienced and haven’t felt anything distinct since I got the monitor. What I’m feeling is very occasional, subtle “sensations”…but these may turn out to be nothing. I’m okay with that. As a matter of fact, I’m not even worried about what the data might show.
I just want this thing off me.